Keratoconus
Keratoconus is a condition in which the cornea becomes conical. The cornea is the transparent layer in front of the eye orbit. If we analogize human orbit eye to the lights of the car, cornea can be considered as the glass of the light. Normally, the corneal shape is spherical and regular which passes the light such as a convex lens and create a clear image on the retina. However, in keratoconus, the corneal shape changes into conical, and it can be stated that it becomes “cony” or “humpy”, and also irregular and uneven. This problem impairs development of a clear image of the object in the eyes, and the person experiences blurred vision.
What are the causes of keratoconus?
In most cases, this disease has no causes, which begins to develop during adolescence and progresses over time. Therefore, keratoconus, unlike cataract is a disease for the youth and teenagers. Rarely, genetic and environmental factors may be involved in its development. Nevertheless, in individuals with severe high-sensitivity and those who rub their eyes frequently there is a chance for development of this disease as well.
Is keratoconus considered a dangerous disease which can culminate in blindness?
No. Fortunately, in keratoconus only corneal is involved and other sensitive layers of the eyes including lens, retina, and nerves of the eyes are normal. Even if the disease progresses to its ultimate state, it never ends in blindness and after the treatment typically the person regains its vision.
What is the treatment for keratoconus?
The treatment of this disease is dependent on its degree of severity as well as age of the patient and their vision status. In very mild cases where the patient does not feel much problem and has relatively good vision, there is no need to any special measures and the patient should be followed up. However, for cases when diminished vision is observed, usually glasses are prescribed and with glasses their vision is corrected. In more advanced cases when the patient does not resolve with glasses, one can use contact lenses. These types of lenses are rigid and with the training given to the patient they can place the lenses in their eyes or remove them. Typically, these lenses should be removed during night and before sleep. Adhering to recommendations of the ophthalmologist and taking proper care of lenses and the always can prevent complications of these lenses.
Hybrid soft and mini-scleral lenses
In the past, for treating keratoconus using contact lenses, there are some limitations and only typical rigid lenses were available. Some patients did not tolerate these lenses, and in those who the disease has been aggravated, these lenses could not be well placed and fit on the cornea. Today, more advanced types of these lenses are available and it is possible for a larger number of patients to use this lens. Some of these lenses are a combination of soft and rigid lenses which are known as hybrid lenses. Some others have a special shape and design which are larger such that they are embedded on the sclera, and as such they are called scleral and mini-scleral. In Parsian clinic, the ophthalmologists prescribe and order different types of these lenses based on the corneal situation of patients.
When surgery is required?
Although surgery brings about favorable outcomes, it is recommended only when the patient does not find a good vision with glasses and cannot use lenses. Even it is recommended that in case the patient had used lens previously, their lenses should be investigated again and if required newer lenses should be prescribed for them. However, if the patient cannot use lenses for any reason and does not have a good vision with glasses, inevitably they will be a candidate for surgery.
What are the operations that are done for keratoconus?
There are different types of surgery for this disease, where the most common are intra-corneal rings and corneal transplantation. Recently, various therapeutic laser techniques including PRK and trans have been used in some patients. Cross-linking by UV is one of the new methods which is used for these patients.
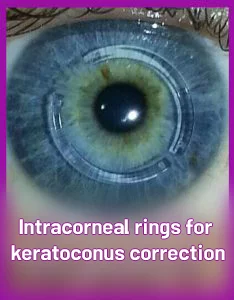
Intracorneal Rings
Intracorneal rings are rings which are embedded to correct some deceases inside the corneal tissue and with transforming the cornea, they improve the vision of the patient. These rings are usually used today for correcting keratoconus. The diameter of these rings varies between 5 and 7 mm, which are available as two-pieced or a complete ring. Their thickness is also different (150-450 micron) and their diameter and thickness are chosen based on the severity of disease. For their incorporation, special mechanical devices and today mostly Femtosecond laser device are used. After creating one or two channels in the depth of the cornea, one piece or two pieces of the ring are placed inside the channel and with the pressure exerted in the corneal tissue, it causes more regularity of the corneal surface and correction of vision. To embed the complete ring, a round cut should be made inside the cornea as a pocket.
Selection of the type of rings, as well as their thickness and diameter are dependent on the status of the corneal disease as well as the taste and experience of the ophthalmologist. Nowadays, different types of these rings are offered in Parsian clinic using the advanced technology of Femtosecond laser.
Corneal transplantation
The most effective operation for patients with severe keratoconus is corneal transplantation. In the past, this transplantation was performed on the entire thickness of the cornea. However, since the internal layer of cornea which plays a sensitive role in the transparency of cornea is normal in these patients, today attempts are made to perform the operation as ‘lamellar” or half-thickness, whereby only the front layer of the cornea is removed and transplanted, while its internal layer remains intact. This technique causes a significant reduction in corneal transplant rejection, as the remaining internal layer does not experience rejection. Nevertheless, this technique cannot be used on all individuals and can be performed in 70 to 90% of cases.
The outcome of the transplantation is relatively good and its success rate is high. Nevertheless, it should be noted that some individuals after the operation experience myopia and high astigmatism, necessitating another surgery. Furthermore, a small percentage of individuals may experience rejection and require pharmacotherapy. Then in case of lack of response, they may need re-transplantation. The possibility of rejection is higher during the first months and years and over time its probability diminishes. Nevertheless, it should be stated that if the patient refers to the physician immediately after that rejection, most probably their cornea returns to its normal state with pharmacotherapy. Therefore, patients who have been transplanted are recommended to immediately refer to ophthalmologist or emergency centers of ophthalmology in case of feeling any blurred vision, redness, and eye discomfort.
Corneal transplantation is not equal to eliminating glasses, and these patients may need glasses or operations for vision correction after the surgery.
In Persian Eye Clinic, we use femtosecond laser device for performing the corneal transplantation. Using this device, we would be able to perform the surgery with the proper method which best suits every patient.
Is there any method for preventing keratoconus or halting its progression?
Cross-linking operation by UV radiation (CXL)
As mentioned earlier, using UV radiation, one can halt the progression of the disease. CXL is a new method and we used it for the first time in Parsian clinic. In this method, through radiating rays on the corneal surface, a link is developed between the collagens of cornea and that strength of corneal grows. Currently, this method is used in individuals whose keratoconus is progressing.